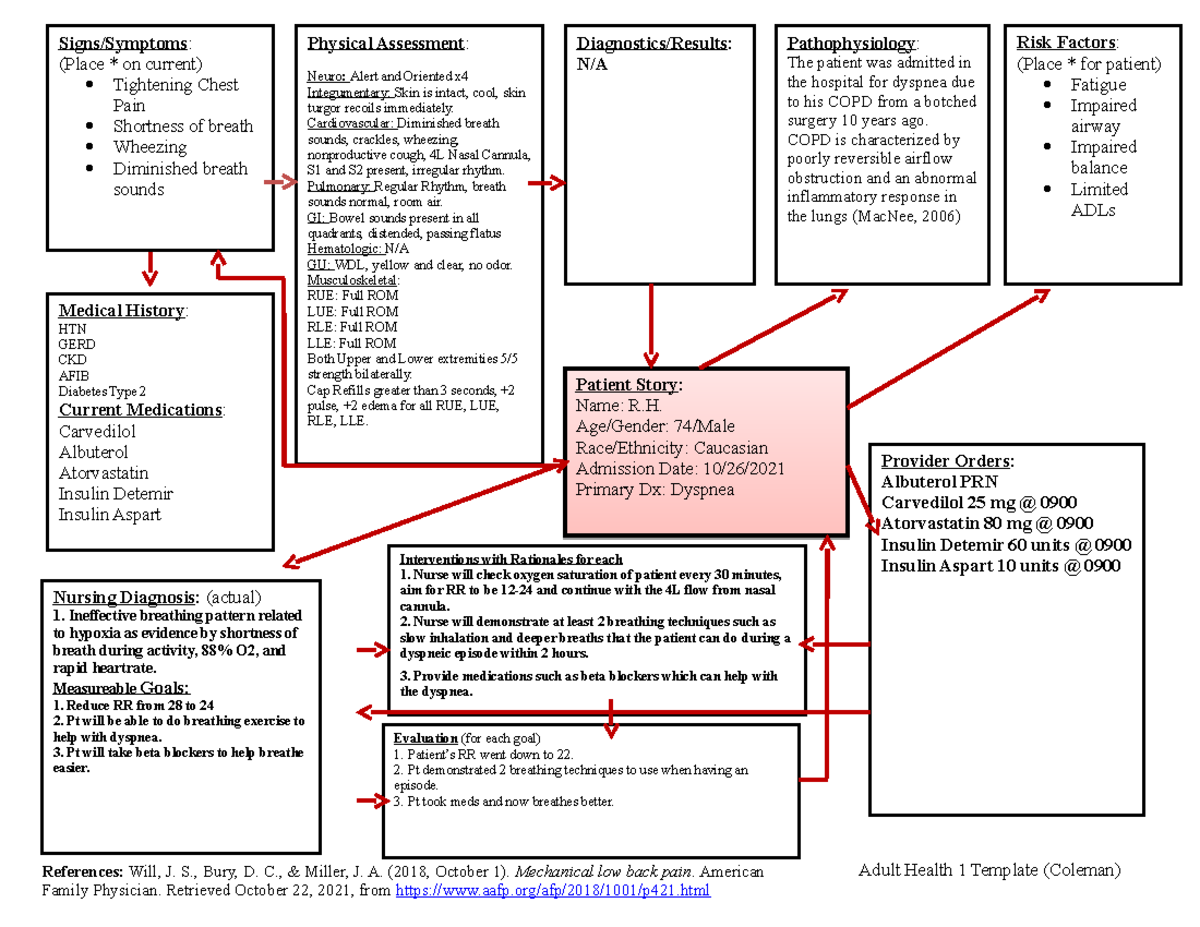
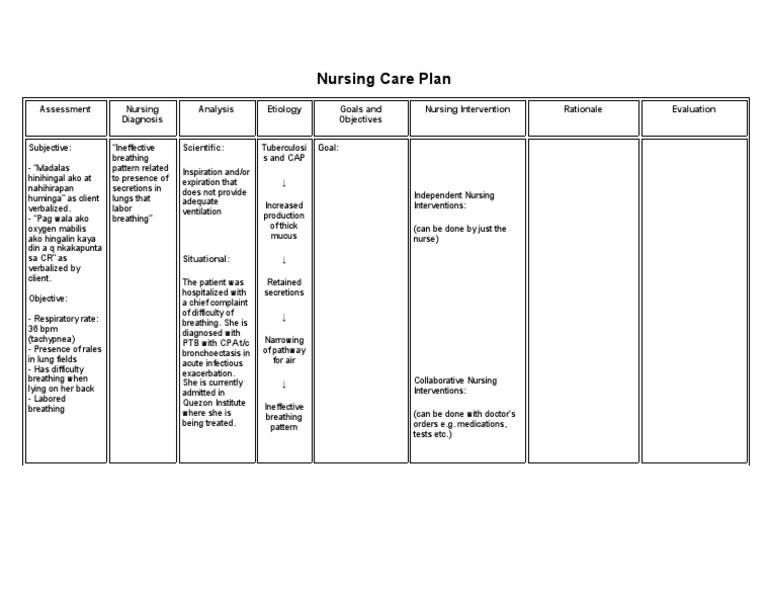
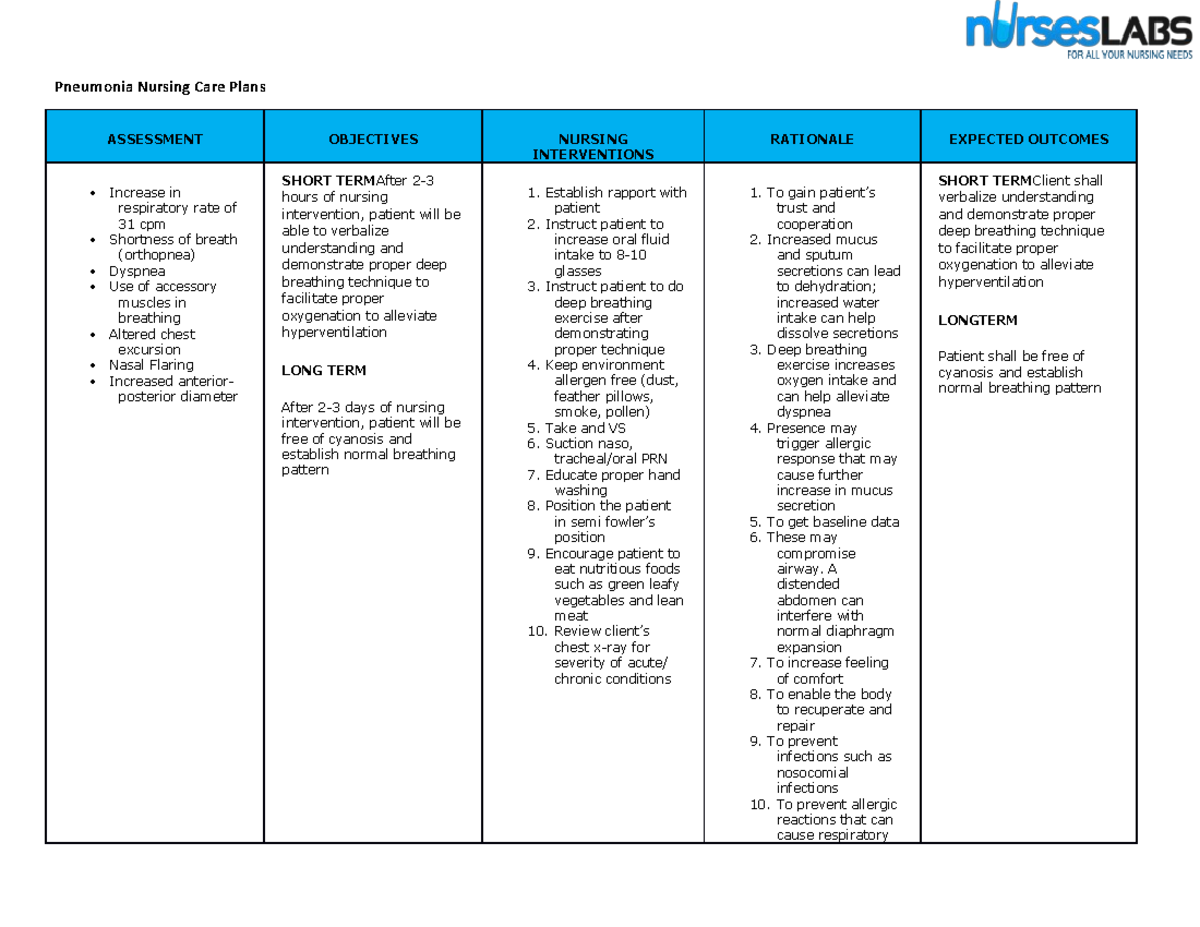
Nursing Goals For Ineffective Breathing Pattern
Nursing Goals For Ineffective Breathing Pattern - (nurse assesses) altered respiratory patterns. The primary goal is to improve oxygenation and ensure adequate gas. Include evidenced based rationales for each nursing intervention using your textbooks. Web goals and expected outcomes for ineffective breathing pattern improved oxygenation: Ineffective airway clearance refers to the inability of the client to effectively clear. Ineffective breathing pattern, dyspnea, respiratory distress. Web the following are common nursing care planning goals and expected outcomes for an ineffective breathing pattern: Listen to respiratory sounds, observe areas of diminished/absent ventilation. Web if you are a nursing student, you will want to fully understand the signs, symptoms, and treatments of ineffective breathing patterns. Patients with sleep apnea experience ineffective breathing patterns as the airways can become obstructed and collapse during. Patient will deny shortness of breath. Listen to respiratory sounds, observe areas of diminished/absent ventilation. Web the short term goals are for the patient to understand their treatment and demonstrate proper breathing techniques to alleviate symptoms. The nursing care planand management for dyspnea or ineffective breathing pattern typically involve assessing the underlying cause, providing immediate and appropriate interventions to alleviate the symptoms, and implementing measures to promote respiratory comfort and overall well. The presence of crackles or rales indicate fluid in. Objective/expected outcome ;the patient will: Include evidenced based rationales for each nursing intervention using your textbooks. Web goals and expected outcomes for ineffective breathing pattern improved oxygenation: The primary goal is to improve oxygenation and ensure adequate gas. Patient will establish an effective breathing pattern as evidenced by abgs and spo2 within normal limits. (nurse assesses) altered respiratory patterns. Web the following are common nursing care planning goals and expected outcomes for an ineffective breathing pattern: Include evidenced based rationales for each nursing intervention using your textbooks. Listen to respiratory sounds, observe areas of diminished/absent ventilation. The primary goal is to improve oxygenation and ensure adequate gas. Web irregular breathing pattern; Patient will establish an effective breathing pattern as evidenced by abgs and spo2 within normal limits. Web an ineffective breathing pattern requires investigation for respiratory infections, lung trauma, chronic airway changes, cancer, etc., to manage effectively. The nursing care planand management for dyspnea or ineffective breathing pattern typically involve assessing the underlying cause, providing immediate and. Web patient to increase breathing capacity. Web the following are common nursing care planning goals and expected outcomes for an ineffective breathing pattern: Include evidenced based rationales for each nursing intervention using your textbooks. State whether or not the goal was met. The long term goals are for the. Listen to respiratory sounds, observe areas of diminished/absent ventilation. Web an ineffective breathing pattern requires investigation for respiratory infections, lung trauma, chronic airway changes, cancer, etc., to manage effectively. The presence of crackles or rales indicate fluid in. The long term goals are for the. Patient will establish an effective breathing pattern as evidenced by abgs and spo2 within normal. Web the short term goals are for the patient to understand their treatment and demonstrate proper breathing techniques to alleviate symptoms. Web the nursing care plan outlines a patient who is experiencing ineffective breathing patterns related to their disease process, with subjective assessments noting tachypnea,. The nursing diagnosis and interventions can help reduce risks associated. The table 1 shows that. This nursing care plan and diagnosis is for the following condition: (nurse assesses) altered respiratory patterns. The primary goal is to improve oxygenation and ensure adequate gas. Web ineffective breathing pattern care plan: Web pressure on the diaphragm. Web an ineffective breathing pattern requires investigation for respiratory infections, lung trauma, chronic airway changes, cancer, etc., to manage effectively. The table 1 shows that ibp was associated with the following dc: The primary goal is to improve oxygenation and ensure adequate gas. Ineffective airway clearance refers to the inability of the client to effectively clear. Web the short term. Include evidenced based rationales for each nursing intervention using your textbooks. Ineffective breathing pattern, dyspnea, respiratory distress. Web an ineffective breathing pattern requires investigation for respiratory infections, lung trauma, chronic airway changes, cancer, etc., to manage effectively. The long term goals are for the. Web irregular breathing pattern; State whether or not the goal was met. The primary goal is to improve oxygenation and ensure adequate gas. Patient will establish an effective breathing pattern as evidenced by abgs and spo2 within normal limits. The table 1 shows that ibp was associated with the following dc: Objective/expected outcome ;the patient will: The table 1 shows that ibp was associated with the following dc: Web nursing care plan for ineffective breathing pattern. (nurse assesses) altered respiratory patterns. State whether or not the goal was met. Web if you are a nursing student, you will want to fully understand the signs, symptoms, and treatments of ineffective breathing patterns. Ineffective breathing pattern, dyspnea, respiratory distress. Web the following are common nursing care planning goals and expected outcomes for an ineffective breathing pattern: The long term goals are for the. Ineffective airway clearance refers to the inability of the client to effectively clear. Web an ineffective breathing pattern requires investigation for respiratory infections, lung trauma, chronic airway changes, cancer, etc., to manage effectively. Web nursing care plan for ineffective breathing pattern. This nursing care plan and diagnosis is for the following condition: (nurse assesses) altered respiratory patterns. The primary goal is to improve oxygenation and ensure adequate gas. Listen to respiratory sounds, observe areas of diminished/absent ventilation. Web if you are a nursing student, you will want to fully understand the signs, symptoms, and treatments of ineffective breathing patterns. Objective/expected outcome ;the patient will: Web pressure on the diaphragm. Web goals and expected outcomes for ineffective breathing pattern improved oxygenation: Patient will deny shortness of breath. The nursing diagnosis and interventions can help reduce risks associated.Ineffective breathing concept map notes **Interventions with
Nursing Care Plan Ineffective Breathing Pattern
Nursing Care Plan for Ineffective Airway Clearance Respiratory Tract
NCP Ineffective Breathing Pattern Tala
Ineffective Breathing Pattern Nursing Diagnosis and Nursing Care Plan
Ineffective Breathing Pattern Breathing Respiratory System
NCP ineffective breathing pattern
SOLUTION Nursing care plan ineffective breathing pattern poliomyelitis
Nursing Care Plan Ineffective Breathing Pattern
Nursing Care Plan For Ineffective Breathing
Web Irregular Breathing Pattern;
The Presence Of Crackles Or Rales Indicate Fluid In.
Web The Short Term Goals Are For The Patient To Understand Their Treatment And Demonstrate Proper Breathing Techniques To Alleviate Symptoms.
Patient Will Establish An Effective Breathing Pattern As Evidenced By Abgs And Spo2 Within Normal Limits.
Related Post: